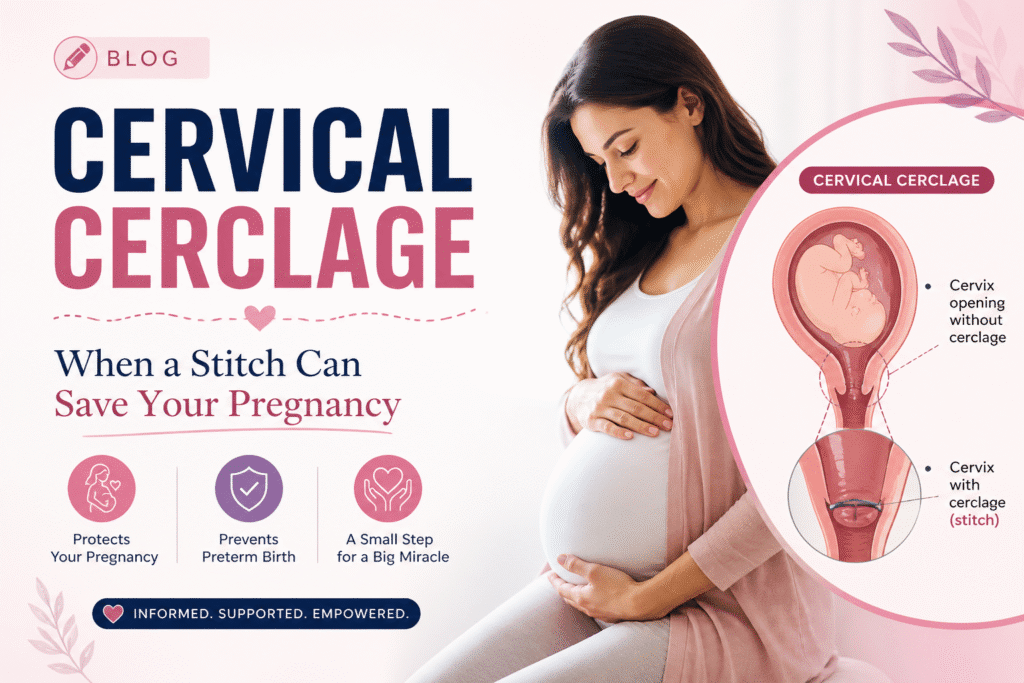
Cervical Cerclage: When a Stitch Can Save Your Pregnancy
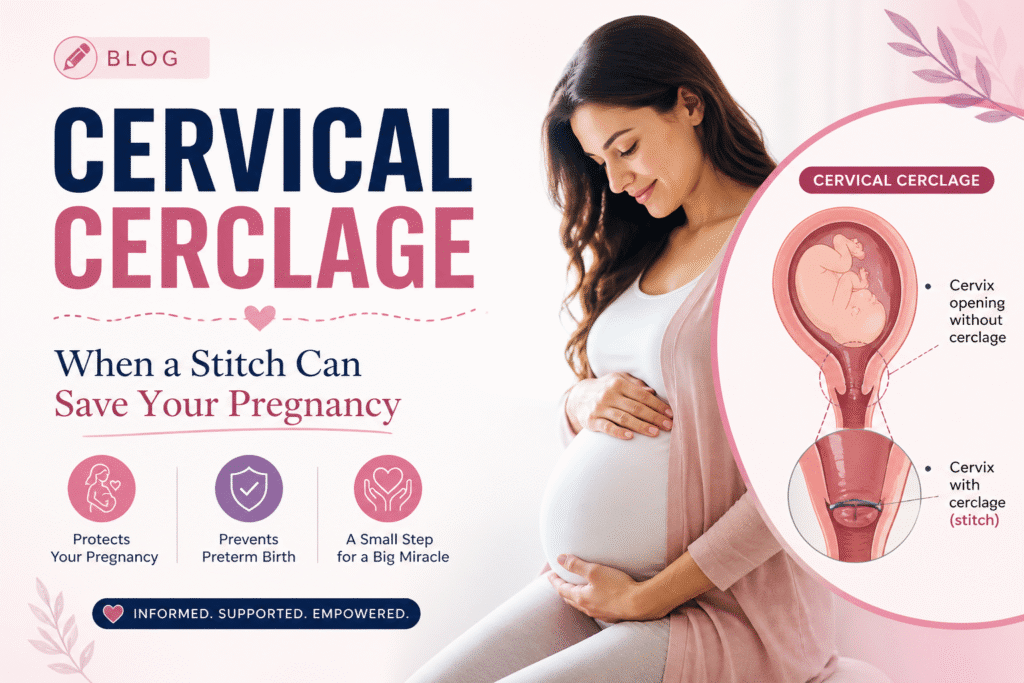
For a woman who has lost a pregnancy after the first trimester, the experience leaves more than just physical recovery. It leaves a quiet fear that whispers, “What if it happens again?” If a doctor has ever told you that you have a “weak cervix” or a “short cervix,” you may already know that fear well.
Here is what often goes unsaid. In many of these situations, there is a small, time-tested procedure that can quietly change the outcome of your next pregnancy. It is called cervical cerclage — a simple stitch placed around the cervix that helps it stay closed until your baby is ready to be born.
This guide walks you through everything you need to know about cervical cerclage in plain language. Who needs it, how it is done, what recovery looks like, and what kind of success you can realistically expect.
What is Cervical Cerclage?
Cervical cerclage is a small surgical procedure in which a strong stitch (suture) is placed around the cervix to keep it firmly closed during pregnancy. The cervix is the narrow opening at the lower end of the uterus, and during a healthy pregnancy it should stay long, firm, and shut until labour begins.
In some women, the cervix is weaker than it should be and starts to open too early — sometimes as early as the fourth or fifth month, often without any pain at all. This is called cervical insufficiency, or in older language, an “incompetent cervix.”
A cervical cerclage works like a drawstring around the neck of a bag. It gives the cervix the mechanical support it needs to hold the pregnancy until the baby is mature enough to be delivered safely.
In simple terms, it is a stitch in the pregnancy cervix that buys your baby precious time to grow. For carefully selected women, it is the most reliable cervical insufficiency treatment available today.
Why is Cervical Cerclage Needed?
Your obstetrician may suggest a cerclage if you have one or more of the following:
- Two or more previous miscarriages between 14 and 24 weeks of pregnancy, particularly if the cervix opened painlessly
- A previous very preterm delivery before 34 weeks linked to a short or opening cervix
- A short cervix (less than 25 mm) detected on ultrasound before 24 weeks of the current pregnancy
- Previous cervical surgery such as LEEP, cone biopsy, or repeated D&C, which may have weakened the cervix
- Congenital abnormalities of the uterus or cervix
- A current pregnancy in which the cervix is found to be opening on examination, sometimes with the bag of waters bulging — this is the situation in which a rescue cerclage is considered
If any of these apply to you, this is the right time to talk to a specialist. Short cervix treatment works best when it is started early — and the earlier you are evaluated, the better the outcome tends to be.
Have you had a second-trimester loss, or been told you have a short cervix? Do not wait for the next pregnancy to figure things out. Book your consultation today and get a clear, personalised plan from a specialist in high-risk pregnancy care.
Types of Cervical Cerclage
Not every cervix and not every patient is the same. There are three main types of cervical cerclage, and the right one depends on your history, the stage of pregnancy, and the condition of your cervix.
1. Prophylactic Cerclage (the Planned Stitch)
This is a planned procedure, usually performed between 12 and 14 weeks of pregnancy. It is offered to women with a clear history of cervical insufficiency — typically two or more painless second-trimester losses. Because it is placed before any cervical changes begin, it has the highest success rate of all cerclage types.
2. Rescue Cerclage (the Emergency Stitch)
This is performed when a woman comes in during the second trimester with the cervix already opening, sometimes with the bag of waters visible. It is technically more demanding and time-sensitive, but in experienced hands it can still save many of these pregnancies.
If you have been told that your cervix is opening at 20 to 24 weeks, please understand that it is not necessarily too late — but every hour matters. Reach out to a specialist immediately.
3. Laparoscopic Cervico-Isthmic Cerclage (the Advanced Abdominal Stitch)
This is the most advanced form of cerclage, reserved for selected complex cases — for example, when a previous vaginal cerclage has failed, when the cervix is too short or has been surgically removed, or when the anatomy does not allow a safe vaginal stitch.
Instead of being placed through the vagina, the stitch is placed laparoscopically — through small keyhole incisions in the abdomen — at the very top of the cervix where it joins the uterus. This offers the highest level of mechanical support and is often the best remaining option for women with multiple previous losses.
Laparoscopic cervico-isthmic cerclage is a specialised procedure that requires expertise in both high-risk obstetrics and advanced minimally invasive surgery. We perform this procedure regularly at our centre, both before pregnancy and during early pregnancy, with very encouraging outcomes.
The Cervical Cerclage Procedure, Step by Step
If a vaginal cerclage has been planned for you, here is what to expect.
- Pre-procedure check. A detailed examination, ultrasound, and basic tests to confirm a healthy ongoing pregnancy and to rule out infection.
- Hospital admission. You are admitted to the hospital, usually in the morning, and asked not to eat for a few hours before the procedure.
- Anaesthesia. The procedure is done under spinal anaesthesia or short general anaesthesia. You will not feel any pain.
- Placing the stitch. Through the vagina, the obstetrician places a strong stitch around the cervix to close it firmly. The procedure usually takes 20 to 40 minutes.
- Recovery and monitoring. You are observed for a few hours and the baby’s heartbeat is checked.
- Going home. Most women are discharged the next morning.
The laparoscopic cervico-isthmic cerclage procedure follows the same principle but is performed through tiny abdominal incisions under general anaesthesia. It typically takes 60 to 90 minutes, with a hospital stay of 1 to 2 nights.
Recovery and Aftercare
Most women feel completely fine within 2 to 3 days. Light spotting and mild cramping for the first day or two is normal. We typically advise:
- Rest at home for 2 to 3 days, then a gradual return to light activity
- No intercourse for the rest of the pregnancy
- No heavy lifting, vigorous exercise, or long-distance travel
- Continue your usual antenatal supplements and prenatal vitamins
- Attend all follow-up visits, including periodic cervical length scans
Watch carefully for warning signs — bleeding, watery discharge, contractions, foul-smelling discharge, or fever — and contact us immediately if any of these occur.
A cerclage does not mean you must stay in bed for the rest of pregnancy. Most women continue with a normal daily routine with sensible precautions.
When is the Stitch Removed?
For a vaginal cerclage, the stitch is usually removed at around 36 to 37 weeks of pregnancy. Removal is done as an outpatient procedure, takes only a few minutes, and does not require anaesthesia. Once the stitch is out, you can go into normal labour and have a vaginal delivery if everything else is favourable.
If labour starts before the planned removal date, the stitch is taken out urgently to avoid injury to the cervix.
For a laparoscopic cervico-isthmic cerclage, the stitch is usually left in place permanently and delivery is by planned caesarean. The same stitch can also support future pregnancies, which is a unique advantage of this technique.
Success Rates and Outcomes
When done at the right time and for the right reasons, cervical cerclage has excellent outcomes. Reported success rates are broadly:
- Prophylactic (planned) cerclage: 85 to 90 percent of pregnancies reach a viable gestation
- Ultrasound-indicated cerclage for short cervix: 75 to 85 percent
- Rescue cerclage in emergency cases: 50 to 70 percent, depending on how dilated the cervix is at presentation
- Laparoscopic cervico-isthmic cerclage: over 90 percent in carefully selected patients
These figures are general guides. Your specific outcome depends on your history, your anatomy, and how early intervention is offered. The single most powerful predictor is timely evaluation — which is why women with previous pregnancy losses should be reviewed before the next pregnancy, not midway through it.
What are the Risks?
Cervical cerclage is, in general, a safe procedure with low complication rates. Like any surgery, it does carry some risks, and you deserve an honest picture:
- Mild bleeding or spotting for a day or two
- Infection, which is uncommon and treated with antibiotics
- Rupture of the membranes — rare in planned cases, somewhat higher in rescue cases
- Cervical injury, which is very rare in experienced hands
- Stitch displacement, which may need repositioning
In experienced centres, serious complications are uncommon, and for women who genuinely need the procedure the benefit far outweighs these risks. This is exactly why patient selection matters — and why a careful evaluation by an obstetrician with high-risk pregnancy expertise is so important before any cerclage is planned.
Frequently Asked Questions
Is cervical cerclage painful?
The procedure itself is painless because it is performed under spinal or short general anaesthesia. Some mild cramping or spotting for a day or two afterwards is normal. Most women are pleasantly surprised by how comfortable the recovery is.
Will the stitch hurt my baby?
No. The stitch is placed around the cervix, well below the baby. Your baby continues to grow normally above the stitch and is not affected.
Can I have a normal vaginal delivery after a cerclage?
Yes — for a vaginal cerclage. Once the stitch is removed at 36 to 37 weeks, normal labour and a vaginal delivery are possible if your overall pregnancy is favourable. Laparoscopic abdominal cerclage requires a planned caesarean delivery.
What is the cost of cervical cerclage in India?
Costs vary depending on the city, hospital, and type of cerclage (vaginal versus laparoscopic). Most major Indian health insurance policies cover cervical cerclage when it is medically indicated. Our team helps patients with insurance documentation and pre-authorisation.
Can a cerclage prevent every miscarriage?
No procedure can guarantee that, and any doctor who promises it is not being fully honest. What a stitch does, very effectively, is prevent miscarriage and preterm birth caused specifically by a weak or short cervix. Other causes of pregnancy loss need their own evaluation and treatment.
How soon after a previous loss can I plan my next pregnancy with a cerclage?
Most women can be evaluated within 2 to 3 months of a second-trimester loss, and a planned next pregnancy can usually be considered after about 6 months — though this depends on your individual physical and emotional recovery.
I had a failed vaginal cerclage in my last pregnancy. What are my options?
A failed vaginal cerclage is one of the strongest indications for considering a laparoscopic cervico-isthmic cerclage in your next pregnancy. Success rates in this group are significantly higher than simply repeating a vaginal stitch.
A Final Word of Hope
If you have lost a pregnancy in the second trimester, or have been told that your cervix is short or weak, please carry this thought with you — in many cases what happened was not your fault, and it does not have to happen again.
Cervical cerclage is one of the oldest and most quietly successful tools in modern obstetrics. For the right patient, at the right time, in the right hands, it has helped countless women hold on to their babies long enough to bring them safely into the world.
The most important step is also the simplest — a thorough evaluation and a clear plan, ideally before your next pregnancy.
Talk to Our Specialist — Book Your Consultation Today
If you are planning a pregnancy after a previous loss, are currently pregnant with a short cervix, or have been told you may need a stitch, please do not navigate this alone. At Ankur Maternity Home and Clinic, Ahmedabad, we combine high-risk pregnancy expertise with advanced laparoscopic surgical care, including laparoscopic cervico-isthmic cerclage for the most complex cases.
Every week we get only a limited number of consultation slots for high-risk and pre-pregnancy planning cases. If your situation needs attention, please reach out early.
Phone: +91 97267 21111
Email: ankurmaternityhomeclinic@gmail.com
Address: 425, Avani Icon, Haridarshan Cross Road, opp. Shalby Hospital, Nava Naroda, Ahmedabad – 382330
Disclaimer: This article is intended for general educational purposes only and is not a substitute for personalised medical advice. The decision to undergo cervical cerclage must be made in consultation with a qualified obstetrician based on your individual medical history.